Dysregulation of the immune system and autoimmune processes play a key role in severe and long-term course of COVID-19 infections. Research has shown that autoantibodies against phospholipids, anti-cardiolipin and anti-beta-2-glycoprotein, may contribute significantly to COVID-19 related autoimmunity and disease severity. Understanding how these antibodies trigger the thrombotic manifestations of the disease is important to improve patient management and to understand the underlying pathophysiology of SARS-CoV-2 infection.
Doctors’ awareness of autoantibodies promoting COVID-19 disease and determination of these autoantibodies with reliable laboratory tests will benefit the patients.
Category: Allgemein
Biomarkers for disease activity in Crohn’s disease
May measuring of fecal calprotectin replace colonoscopy for follow up of patients with Crohn’s disease after surgery?
After intestinal resection patients with Crohn’s disease need close monitoring and tailored therapy adjustment to reduce the risk of relapses. Today, colonoscopy is still the gold standard for the detection of disease reactivation, an invasive procedure which is unpleasant for the patient and expensive for the health care systems.
Biomarkers in blood or stool samples that correlate with endoscopic findings could therefor improve the surveillance of patients with inflammatory bowel diseases.
A candidate marker for this purpose is measurement of calprotectin concentrations in stool samples from affected patients.
Rheumatoid Factor revisited: An “old” test but still up to date
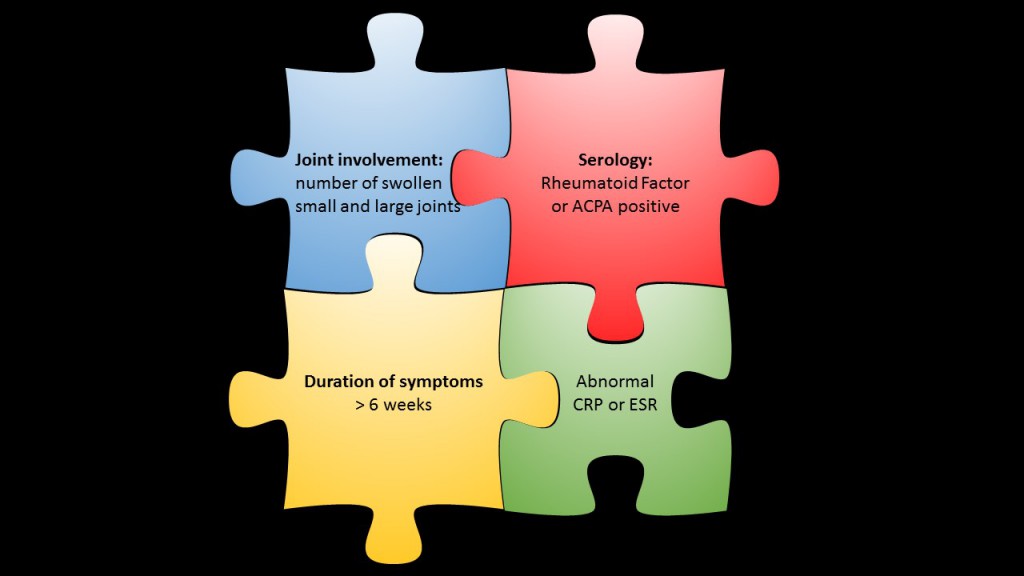
Rheumatoid factor (RF) is one of the best known serological markers in rheumatology – development of the test dates back into the 1940ies. Since this time the toolkit of serological diagnostic tests for rheumatoid arthritis (RA) has been complemented by the more specific anti-citrullinated protein antibody (ACPA) tests. However, none of the various ACPA tests has completly replaced RF until now.
In contrast, the significance of RF has been further substantiated with the definition of the 2010 ACR criteria for classification of RA. Moreover, recent studies have shown the potential of RF as a contributor to disease pathogenesis.
(more…)
The 2012 revised SLICC criteria for classification of systemic lupus erythematosus

The famous musician Seal is known for his numerous international hits, and for living with an autoimmune disease: the scars on his face are the result of discoid lupus erythematosus. Picture: C. Grube for Access2music.de, wikimedia
Systemic lupus erythematosus (SLE) is a chronic inflammatory disease with manifold manifestations. SLE belongs to the family of autoimmune disorders, diseases that occur, when a mislead immune system attacks the body’s own structures. SLE can affect almost any organ system, thus its presentation and course are highly variable, and diagnosis and therapy may be challenging.
With the intention to classify SLE patients for research and surveillance studies and to support clinicians in confirming a diagnosis, a set of clinical and laboratory classification criteria has been developed and released by the American College of Rheumatology (ACR). The first classification criteria for SLE were originally published in 1971 [1,2]. They have been updated 1982 [3] and 1997 [4] to incorporate new immunologic knowledge and improve patient classification. In contrast to the 1987 criteria, the 1997 criteria have not been validated.
The most recent addendum to the classification criteria for SLE dates from 2012, when the Systemic Lupus International Collaborating Clinics (SLICC) group published a revision and validation of the ACR criteria [5].
Research Update: Rheumatic Disease and Pregnancy
![]() Inflammatory rheumatic diseases predominantly affect women. This also includes many young women who would like to have children or who have not yet completed their family planning when they are first diagnosed. These women do not need to give up on their desire to have children forever. Women with rheumatic disease tend to have fewer children than other women, and it often takes them longer to achieve a desired pregnancy. Today, carefully monitored medical treatment and close collaboration between the rheumatologist and the gynaecologist give these women the opportunity to bring a healthy child into the world.
Inflammatory rheumatic diseases predominantly affect women. This also includes many young women who would like to have children or who have not yet completed their family planning when they are first diagnosed. These women do not need to give up on their desire to have children forever. Women with rheumatic disease tend to have fewer children than other women, and it often takes them longer to achieve a desired pregnancy. Today, carefully monitored medical treatment and close collaboration between the rheumatologist and the gynaecologist give these women the opportunity to bring a healthy child into the world.